A fulcrum is defined as the point of support on which a lever turns in moving something up to a higher position (Fulcrum 2017). If we say that nursing diagnosis is the fulcrum of practice competence and excellence, we are saying that it has a very important effect in elevating the quality of our professional nursing practice. 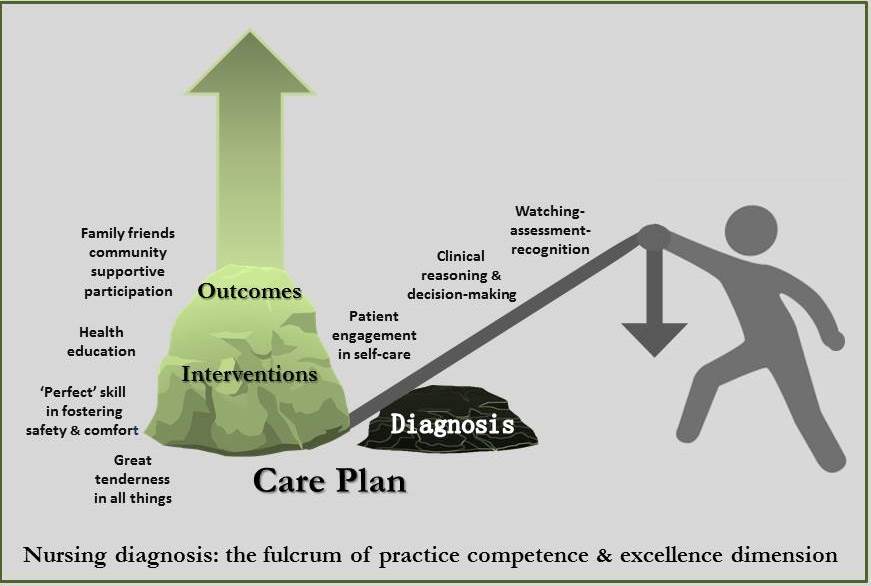
What is a nursing diagnosis?
A nursing diagnosis is 'a clinical judgment concerning a human response to health conditions/life processes, or vulnerability for that response, by an individual, family, group, or community (Gallagher-Lepak, 2014). This is the North American Nursing Diagnosis International (NANDA-I) definition, which we use in Careful Nursing. A nursing diagnosis is different from a medical diagnosis: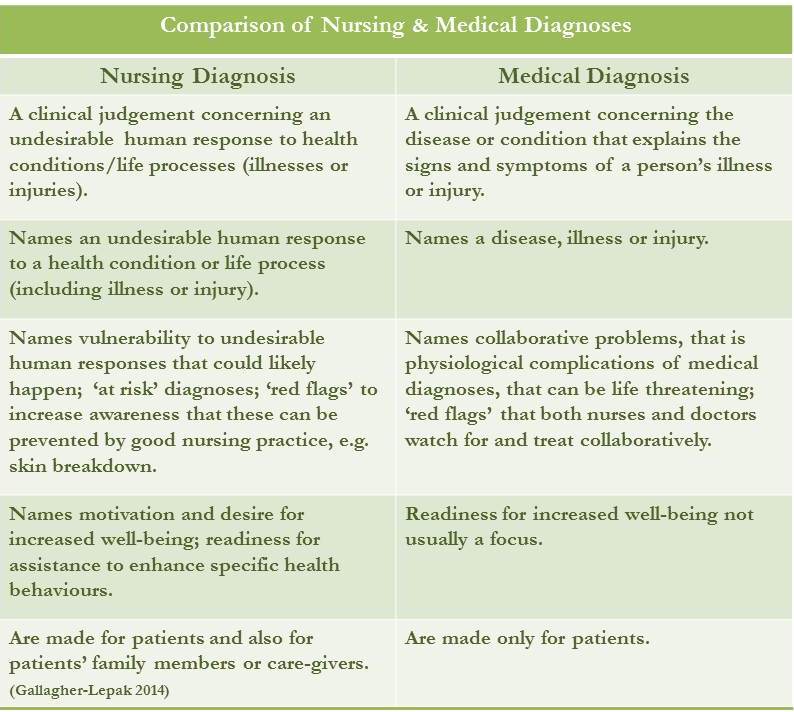 
Why use nursingdiagnosis?
You might be thinking; we have always said nursing problem; it is part of the nursing process. Only doctors make a diagnosis; are we just trying to be like doctors?
No; definitely not.
It is true that the word diagnosis has long been associated with medicine but it does not belong to any particular professional group. The meaning of diagnosis comes from the Greek, diagignoskein which means to "discern, distinguish," literally "to know thoroughly," from dia- "apart" + gignoskein "to learn" (Diagnosis 2017). A diagnosis is a problem that has been thoroughly examined and identified accurately; it can be distinguished from any other problem that looks the same or is similar.
Diagnosis became associated with medicine because different illnesses and injuries share some of the same signs and symptoms and it can be difficult to determine accurately what illness a patient actually has. Accuracy and being able to distinguish one problem from another is essential.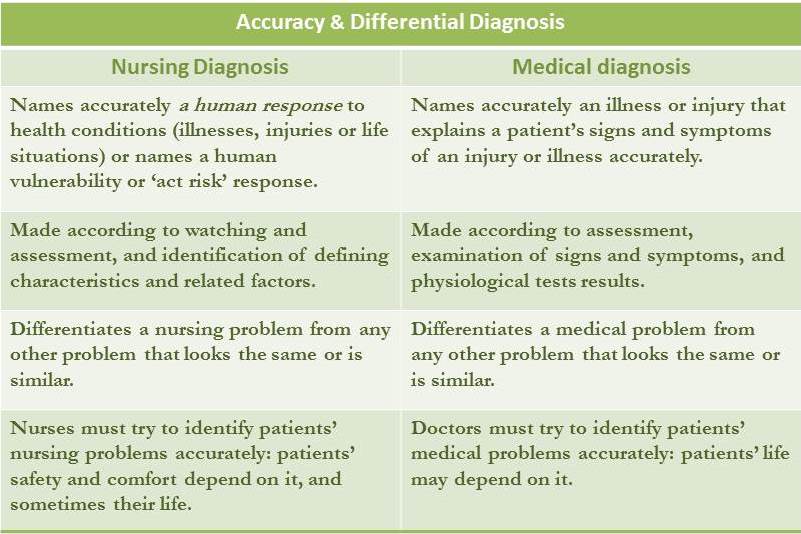 
Accuracy: an essential – a challenge – an opportunity
Aiming for accuracy is essential to enhance the safety and quality of our practice. At the same time, aiming for accuracy is a big challenge because of the complexity of patients' responses to illness, injury and life process situations. But aiming for accuracy is also a big opportunity because it helps us to develop our assessment and critical thinking ability. There is lots of help in the literature, much of which is open to down-load from the web via CINAHL. For example, Lunney (2003, 2010) identifies, discusses and demonstrates seven cognitive skills and ten habits of mind found very useful in developing clinical decision-making and ability to make a nursing diagnosis. Cruz et al. (2009) describe and evaluate a continuing education course concerned with the critical thinking and clinical reasoning needed to improve nursing diagnosis accuracy. A valid and reliable measurement instrument, the Quality of Diagnoses, Interventions, and Outcomes (Q-DIO) developed and tested since 2008, is available to assess the quality of nursing records in any format with regard to nursing diagnosis, interventions and outcomes (Linch et al. 2015).
Nursing diagnoses: the first step
Of course, making a nursing diagnosis is just the first step in developing a nursing care plan. Once the diagnosis is made, an outcome (Morehead et al. 2012) is selected and a baseline measure made. Then nursing interventions (Bulecheck et al. 2013) are selected and outcomes measured regularly.
The 'always' step
In constructing such a nursing care plan the patient is always engaged is the process – patient engagement in self-care – to the extent that this possible for, and desired by, the patient. Naturally, this links to another concept – health education.
Post script: Nursing diagnosis is not new
For various reasons nursing diagnosis may be new to some of us; but it is not new to our profession. Perhaps the earliest use of nursing diagnosis in the literature appeared in The American Journal of Nursing in 1953 when Vera Fry wrote about the importance of taking a creative approach to nursing practice. Following assessment of the individual person's needs, she proposes that:
the first major task in our creative approach to nursing is to formulate a nursing diagnosis and design a plan which is individual and which evolves as a result of a synthesis of needs'(p. 302).
The idea of a nursing diagnosis developed gradually over the following 20 years. Then, in 1972 the expectation that nurses make a nursing diagnosis was included for the first time in a United States Nurse Practice Act, that of New York state; 'diagnosing and treating human responses to actual or potential health problems' became part of the legal domain of professional nursing (Jarrin 2010, p. 167). The North American Nursing Diagnosis Association–International (NANDA-I 2017) took up this creative work and made it global. Along with the Iowa Nursing Outcomes Classification and the Iowa Nursing Interventions Classification, they invite all nurses to join them in this effort which gives us 'words to put on what we do'; thus, it increases our control over our practice, enhances our professional identity, and gives us professional authority.
Just think!
If you are not using nursing diagnoses (NANDA-I 2017), and related outcomes and interventions with enthusiasm to develop, and engage patients' participation in developing, nursing care plans, you are at least 65 years behind the times, and your creativity in nursing practice could be questioned.
References
ReferencesBulechek, G.M., Butcher, H.K., Dochterman, J.M. & Wagner, C. (Eds.). (2013) Nursing Interventions Classification (NIC) (6th ed.). St Louis/London: Mosby/Elsevier.
Cruz, D.M., Pimenta, C.M. & Lunney, M. (2009) Improving critical thinking and clinical reasoning with a continuing education course. The Journal of Continuing Education in Nursing (40) 121-127.
Diagnosis (2017) http://www.etymonline.com/index.php?allowed_in_frame=0&search=diagnosis
Fry, V.F. (1953) The creative approach to nursing. The American Journal of Nursing, (53) 301-302. (Stable URL: http://www.jstor.org/stable/3459609)
Fulcrum (2017) https://www.collinsdictionary.com/dictionary/english/fulcrum
Herdman, T. H. & Kamitsuru, S. (Eds.). (2014) Nursing Diagnoses Definitions and Classifications 2015-2017. Oxford: Wiley Blackwell.Fulcrum (2017)
Gallagher-Lepak, S. (2014) Nursing diagnosis basics. In Herdman, T. H. & Kamitsuru, S. (Eds.). Nursing Diagnoses Definitions and Classifications 2015-2017. Oxford: Wiley Blackwell, 21-30.
Jarrin, O.F. (2010) Core elements of U.S. Nurse Practice Acts and Incorporation of nursing diagnosis language. International Journal of Nursing Terminologies and Classifications (21) 166-176.
Linch, G.F.C., Rabelo-Silva, E.R. & Keenan, G.M (2015) Validation of the Quality of Diagnoses, Interventions, and Outcomes (Q-DIO) instrument for use in Brazil and the United States. International Journal of Nursing Knowledge (26) 19-25.
Lunney, M. (2010) Use of critical thinking in the diagnostic process. International Journal of Nursing Terminologies and Classifications (21) 82-88.
Lunney M. (2003) Critical thinking and accuracy of nurses' diagnosis. International Journal of Nursing Terminologies and Classifications (14) 96-107.
Moorhead, S., Johnson, M., Maas, M.L. & Swanson, E. (2012) Nursing Outcomes Classification (NOC) (5th ed.). St. Louis/London: Mosby/Elsevier.
NANDA-I (2017) http://www.nanda.org/
Therese Meehan
